Pain control is among those skills that specifies the high quality of frontline treatment. When a client is wincing on the floor of a factory, or a child is panicked after a substance fracture at a weekend video game, you don't have lengthy to make audio decisions. PUAEME008, Provide Discomfort Monitoring, codifies what proficient -responders have to do to assess discomfort, select and provide safe analgesia, screen results, and hand over care. It is more than an unit of competency. It is a small between a clinician and a person in distress.
I have provided and evaluated this device for emergency pain management techniques mixed groups, from remote mine medics to urbane event paramedics, and the exact same styles turn up every course: know your pharmacology and contraindications, regard permission and regulation, never forget non‑pharmacological care, and document as if someone else will certainly require to keep up the baton ten mins later on. This post unloads PUAEME008 in practical terms and offers a functioning picture of what competent performance resembles in actual environments.
Where PUAEME008 Sits in Practice
PUAEME008 beings in the general public Security Training Plan and is commonly packaged right into pain administration programs run by signed up training organisations for emergency situation responders and allied wellness professionals working in ascetic or prehospital contexts. Learners are generally already trained in primary study, airway management, basic life assistance, and scene safety and security. The provide discomfort administration training course builds on that structure to address safe, reliable analgesia throughout a range of individuals and environments.
Providers vary across Australia. Some provide the unit as a standalone discomfort management certificate program, others fold it into more comprehensive programs like remote location first -responder training. For registered nurses and physiotherapists that work in occasion medicine, job-related health, or remote outreach, it can complement professional registration by formalising prehospital analgesia skills. It is not a replacement for a tertiary pain fellowship. Rather, it is a concentrated emergency situation discomfort monitoring module that asks an essential concern: can you relieve discomfort swiftly and safely while expecting deterioration?
The Proficiency at a Glance
PUAEME008 assessors try to find clear, evident efficiency. The wording varies slightly throughout variations, yet the core requirements stay secure:
- Recognise and examine acute pain using structured tools suited to the person and situation. Select appropriate analgesic approaches, including non‑pharmacological methods, according to methods, range of practice, and readily available resources. Administer analgesia safely making use of accepted paths, does, and devices while keeping infection control. Monitor reaction, adverse impacts, and important signs, then titrate or cease treatment accordingly. Communicate plainly, gain approval, record, and turn over to a greater level of care.
These components audio tidy theoretically. Actual scenes are not. You will certainly evaluate a person with distracting injuries and a wind blowing sand into your eyes. You will try to find a radial pulse while a group movies on their phones. Capability receives how you develop a fast yet trustworthy image, keep the patient engaged and calm, and apply a method without tunnel vision.
Assessment and Triage: Checking Out Discomfort, Not Presuming It
Pain is subjective and heavily coloured by worry, culture, and context. A jackaroo with a disjointed shoulder may rate his discomfort at six however look pale and clammy with a heart price of 130. A kid might reject to speak however wince with a light touch. PUAEME008 anticipates -responders to utilize pain ranges that fit the client. The numeric rating scale from 0 to 10 fits articulate adults. The Wong‑Baker faces range helps with interaction with kids or patients that choose visual signs. For non‑verbal patients, behavioral devices such as the FLACC range help, though they require practice to prevent overcalling distress as pain.
Acute discomfort evaluation in the field need to not wander right into a lengthy interview. Anchor it within the primary and additional studies. Begin with life hazards, after that a focused discomfort history: place, beginning, character, radiation, severity, time course, worsening or soothing factors, and previous analgesics. Pulse oximetry, heart rate, breathing price, blood pressure, and skin signs provide context. Note warnings that transform the plan: modified psychological state, thought major hemorrhage, breast discomfort with hemodynamic instability, serious head injury, or signs of blood poisoning. PUAEME008 wants responders to identify when analgesia is necessary and when support of airway, breathing, and circulation has to precede it by minutes that really feel much longer.
Anecdotally, the most usual analysis error from brand-new learners is stopping working to reassess. They record a standard pain score, deliver an opioid, after that go on with other tasks. 10 mins later the pain has held one's ground, but because no structured reassessment occurred, the possibility to titrate is lost. Good technique is simple. Tape a pain rating before therapy, however every 5 to 10 mins or after each dosage. Combine it with vitals and an observation of sedation level, so you can find breathing clinical depression early.
Pharmacological Options: What's in the Set and When to Use It
The offer pain management training course shows pharmacological options aligned to organisational protocols. Schedule differs. Remote facilities may stock methoxyflurane, intranasal fentanyl, paracetamol, and advil. Event medics may run under standing orders for oral anesthetics just. Paramedic solutions add IV morphine, ketamine, and occasionally nitrous oxide.
Paracetamol stays the quiet workhorse. At therapeutic doses it reduces pain in musculoskeletal injuries and soft cells injury. It likewise pairs well with NSAIDs for a collaborating result. Look for current intake to prevent advancing toxicity, particularly in smaller grownups or those with liver disease. Advil and various other NSAIDs bring anti‑inflammatory advantages however carry blood loss and kidney dangers. Post‑operative people, the elderly with bad kidney get, and people on anticoagulants may be better offered by alternate strategies.
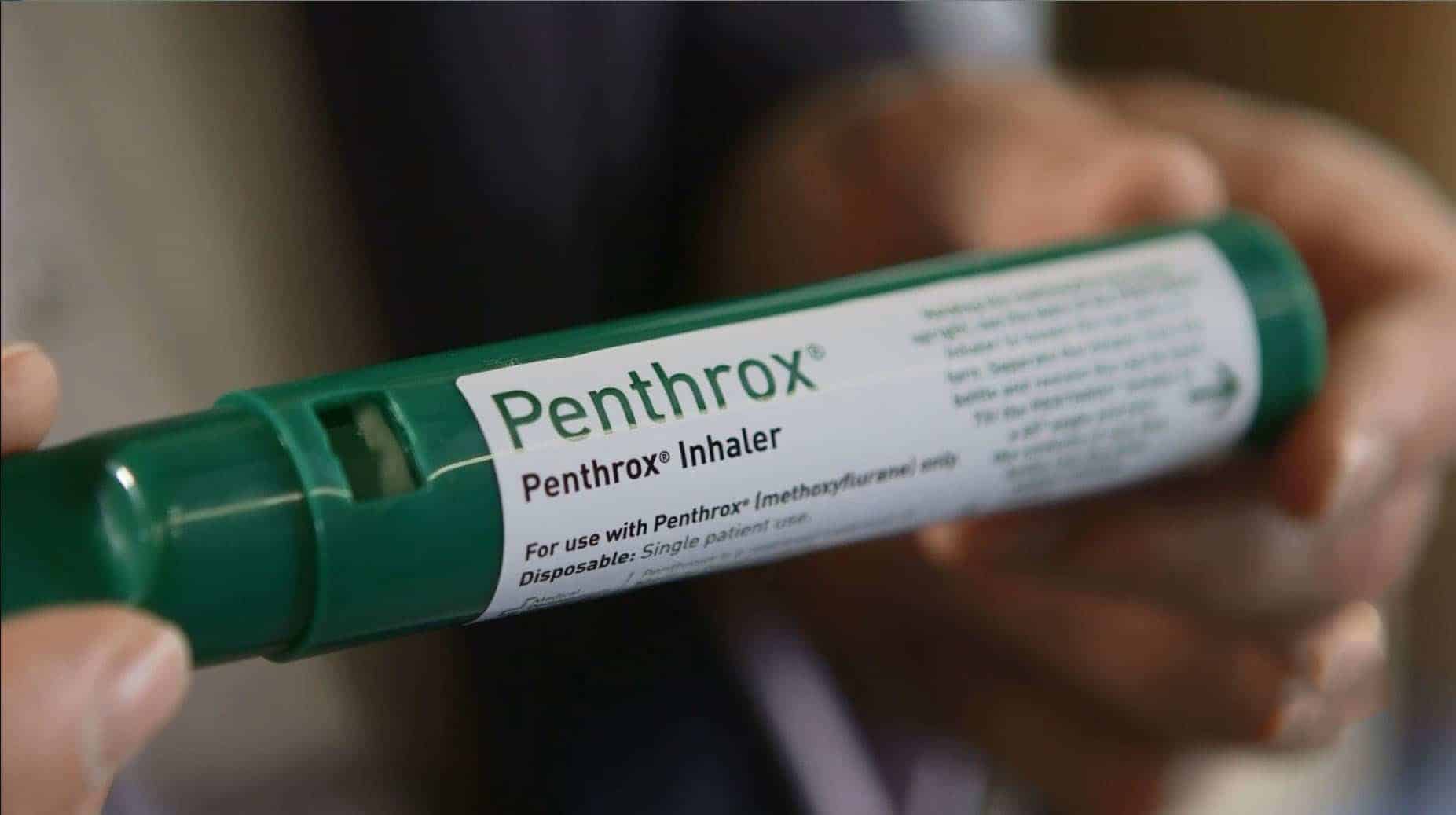
Methoxyflurane, delivered by means of a handheld inhaler, has a faithful following in the area. Its quick onset and patient‑controlled nature fit short, painful procedures like reducing a disjointed shoulder or splinting a crack. Watch for sedation, hypotension, and the collective dosage limit. Many procedures top it at two 3 millilitre vials in 1 day. I have actually had people that hardly touched the inhaler after the initial min because concentrated mentoring and splinting alleviated. Others needed the full allowance to promote extrication. It is appealing to push ahead with techniques while the client is calm, however if their vitals trend improperly, quit and reassess before continuing.
Intranasal fentanyl bridges a key gap when IV accessibility is not possible. Right application based on client weight and delivery through a mucosal atomisation gadget returns quick analgesia. It is especially useful in paediatrics where cannulation delays care. Despite the comfort, treat it with the regard you would any opioid. Know your contraindications, monitor respiration, and have naloxone ready, prepared, and around. Two percent of students fail to remember to prime the atomiser during simulations, which decreases efficacy. Construct a behavior of a fast tools checklist prior to administration.
IV opioids continue to be staples for lots of services. Titrated increments of morphine or fentanyl enable precise control. I like small boluses connected to repeated pain scores and sedation analyses rather than large front‑loaded dosages, particularly for older grownups. Ketamine provides a dissociative course for severe discomfort, specifically in injury where hypotension looms. Reduced dosage ketamine for analgesia varies from induction doses made use of in procedural sedation. Nystagmus and dissociation can unsettle the patient and onlookers, so thorough pre‑briefing aids. I have actually discovered that tranquil narration throughout management reduces the possibility the person will worry as the medication takes effect.
Nitrous oxide still appears at some occasions. It is exceptional for brief, sharp treatments, yet logistics and contraindications complicate its use. Expectant clients, those with bowel blockage, pneumothorax, or trapped gas issues ought to not obtain it. Cylinder administration at a crowded site ends up being a secondary danger otherwise controlled.
Whichever agents you bring, PUAEME008 supports technique in clear protocols and extent. Do not improvisate past training and authorisation, also when stress places. If your discomfort monitoring training program covered intranasal fentanyl and you function under a contract that permits it, you get on solid ground. If ketamine is not in your technique model, the best choice is to intensify or seek extra assistance, not to press boundaries.
Non pharmacological Methods: Often Faster, Constantly Cheaper
I have watched a distressed patient's pain decline from 8 to four within 2 minutes with absolutely nothing greater than a good splint, a cozy covering, and controlled breathing. We speak about drugs because they feel like activity, but fundamental procedures matter.
Immobilisation and splinting stay the most powerful non‑drug treatments for trauma pain. Effectively padded, well positioned splints reduce movement and muscular tissue convulsion. Mild traction in suspected lengthy bone fractures can eliminate the worst of it even before conclusive treatment. Cold treatment reduces swelling and numbs shallow tissues when made use of judiciously. Warmth can help muscle spasm, yet prevent it on fresh stressful injuries.
Positioning slides under the radar. A person with kidney stone discomfort typically finds alleviation curled on one side. Rib cracks really feel better with the upper body a little raised and sustained. Motivate placements that decrease muscle pressure, supplied spine injury is not thought. Easy breathing coaching reduces sympathetic drive and raises resistance. I make use of a 3 count in, six pass over rhythm to promote parasympathetic tone, tuned to the client's comfort. Add distraction. Guided imagery sounds soft until you see a youngster with a lower arm crack settle enough for cannulation due to the fact that you inquired about their canine and the next football match.
Non pharmacological treatment is where physiotherapists and nurses bring huge worth. Discomfort management training courses for physiotherapists frequently emphasise activity approaches that minimize pain without surging stress and anxiety, and registered nurses bring a second sight for placing and confidence that pays rewards. PUAEME008 expects -responders to show these measures alongside pharmacology, not as a consolation reward when the medication kit is light.
Consent, Communication, and Social Safety
Consent can not be a rushed checkbox. Virtually every field mistake I have actually examined after a damaging response included poor pre‑briefing. Before you deliver any type of analgesia, describe what you plan to do, why, what the individual may feel, and what adverse effects to expect, after that request for authorization. Grownups with capability can refuse pain alleviation even if you think it remains in their passion. Paper the conversation.
Cultural security matters. Avoid assumptions about pain expression. Some patients will underreport discomfort to satisfy viewed expectations. Using neutral, open language aids. Rather than asking "Is it a 10 out of 10?", attempt "Can you reveal me on this range how solid the pain really feels today?" For Very first Nations people, invite an assistance individual when possible and bear in mind gendered treatment choices in some communities. Time spent gaining trust fund is rarely squandered and typically shortens the total time to efficient relief since the person engages with your plan.
Paediatrics and older grownups need special attention. With children, authorization includes moms and dads or guardians, however the youngster is entitled to an age‑appropriate explanation and assent. Older adults metabolise drugs differently, and polypharmacy boosts danger. Halve the preliminary dosage, titrate slowly, and keep a hawk's eye on respiration. I have actually stood in lengthy transport lines up during heatwaves where a tiny second dose of an opioid tipped a sickly person from comfy to precariously sleepy. Protocols commonly permit half dosages for older grownups. Use that flexibility.
Monitoring and Handling Adverse Effects
Monitoring is the spine of secure analgesia. Document standard vitals and repeat at periods matched to the medicine's onset and peak. Opioids demand respiration rate and depth checks, oxygen saturation patterns, indicators of air passage blockage, and sedation degree. Ketamine calls for blood pressure, heart price, nystagmus monitoring, introduction responses, and nausea or vomiting. Methoxyflurane requires attention to degree of awareness and high blood pressure. Non‑opioid representatives are not freebies. NSAIDs lug GI bleeding and kidney anxiety risk, though these arise over much longer perspectives. Watch for allergy with any type of agent.
Adverse impacts happen, even with perfect strategy. The metric of competence is not preventing every occasion. It is recognition and decisive management. If a client comes to be extremely sedated after fentanyl, quit dosing, support the respiratory tract, apply extra oxygen, and ready bag‑valve‑mask support. If ventilation is poor or oxygen saturation falls despite respiratory tract maneuvers, make use of naloxone per procedure. I show students to pre‑calculate the naloxone dose for their client immediately after carrying out an opioid, and to verbalise the area of the ampoule. Under stress, this small practice maintains your action measured instead of frantic.
Nausea is common, especially with opioids and methoxyflurane. Have antiemetics obtainable and place a vomit bag in the patient's hands. Lightheadedness and orthostatic drops in stress usually resolve with placing and fluids, if methods enable. Watch on the clock. Drugs have fifty percent lives, and transportation times can be misleading. If you carry out analgesia right before handover, communicate that explicitly so the obtaining medical professional comprehends the timing and can anticipate the next reassessment window.
Documentation and Handover: The Story Has To Travel
Good notes make you a better clinician. Poor ones erode depend on and continuity. For PUAEME008, documents suggests the discomfort assessment tool used and scores in time, the medicines carried out with dose, route, and time, the individual's feedback, negative impacts and actions taken, approval conversations, and non‑pharmacological actions. It additionally indicates context: mechanism of injury, position located, and any kind of obstacles or delays.
Handover gain from an easy structure. I favour an adjusted IMIST‑AMBO approach for pain: Recognition, Mechanism, Injuries/illness, Indications consisting of pain ratings and vitals, Treatment offered (both non‑pharm and medicinal), and action. If the obtaining group listens to that you titrated 20 micrograms of intranasal fentanyl to a paediatric forearm crack, with pain decreasing from 8 to three, and that the youngster remained sharp with stable vitals and no nausea or vomiting, they promptly understand where to pick up.
Training Pathways and That Benefits
Pain administration training comes in different flavours. Brief programs in pain monitoring packaged around PUAEME008 generally run 1 to 2 days, with a balance of concept, simulation, and useful assessment. Some suppliers include optional components like nitrous oxide handling, or innovative splinting. A certificate program in pain administration at this level does not provide authoritative authority by itself. It validates competence to deliver analgesia within an organisation's medical governance and standing orders.
For nurses that grab shifts in occasion medicine or run in rural clinics, pain monitoring courses for nurses help equate hospital‑based skills into prehospital restraints. Emphasis falls on minimal sources, solo decision making, and documents that creases efficiently into rescue or retrieval handover. Physiotherapists functioning pitch‑side or in remote outreach add worth with biomechanics and mild motion strategies. Discomfort management programs for physiotherapists educate just how to combine those strengths with risk-free analgesic methods when doctors are not quickly available.
Paramedic pupils often come across PUAEME008 integrated right into their more comprehensive program. For initial -responders in the resources field, a provide discomfort administration program might be a licensing demand before being rostered to solo coverage. The pragmatic benefit is clear. When I compare incident records prior to and after staff complete a pain management accreditation training course, I consistently see faster time to very first analgesia and less unintended unfavorable occasions. The act of practicing permission scripts, rehearsing dosing, and memorizing red flags modifications behavior under stress.
Equipment and Atmosphere: Information That Matter
You do not need a medical facility to supply excellent pain care, yet you do require reliable set and a system that keeps it ready. Stock checklists conserve careers. Inhalers expired last month help no one. Atomisers that do not fit your syringes hinder strategies. Include human variables. A dim arena tunnel without a headlamp turns creating medication right into a high-risk game. A windy roadside strips warmth from a semi‑dressed individual and presses their pain up while you prepare a line. Small touches obtain ignored up until they bite. I position a thermal covering under and over injury patients whenever possible, after that reassess pain prior to I reach for drugs.


Storage and safety matter. Opioids require locked storage and mindful audit. Maintain a tamper‑evident system and train every employee to utilize it similarly. Naloxone must sit near opioids, not buried in a separate pouch. I have seen groups maintain it in an anaphylaxis package two zips away from the fentanyl. During a dilemma, those zips end up being canyons.
Finally, rehearse where you stand. In confined changing areas, determine beforehand that attracts, who holds, who files. Simulation with full gear deserves an hour of slides. The very first time you attempt to titrate ketamine while a demonstrator's good friends crowd the doorway ought to not be the first time you realise your screen cable television is as well brief for that corner.
Legal and Ethical Boundaries
PUAEME008 presumes technique within a governance structure. Administrative guidelines and organisational protocols specify which representatives you can utilize, under what problems, and with what oversight. Pain administration qualification does not license you to experiment. It verifies you can use a specified method safely. Maintain copies of your range of practice, standing medication orders, and damaging event rise pathway obtainable. If you work across organisations, expect variation. One company may permit intranasal fentanyl under a clinical technique guideline. One more might restrict your analgesia to dental agents and methoxyflurane.
Ethics surface most dramatically when individuals refuse treatment, when spectators push you to rush, or when a coworker prompts a shortcut that sneaks beyond protocol. Your anchor is the mix of patient autonomy, notified permission, and non‑maleficence. Decline to provide a drug if contraindications exist, even if the individual insists. On the other side, do not hold back analgesia as a bargaining chip for participation. Straighten with the receiving service early when you expect complicated choices. A quick phone consult buys medical and lawful cover.
Building Proficiency: What High Quality Training Looks Like
Not all pain administration training courses cover the exact same ground. Search for programs that stabilize pharmacology with situation time, consist of devices taking care of drills, and need demonstration of permission discussions. A great provide pain administration course consists of:
- Realistic simulations that test evaluation, medicine preparation, surveillance, and handover with time pressure. Coverage of non‑pharmacological approaches together with pharmacology, with sensible splinting drills. Clear web links to protocols and extent, including paperwork design templates and adverse event management. Paediatric and older adult considerations, with dosing variations and interaction techniques. Assessment that includes repeated reviews over a circumstance, not simply a solitary dosage and done.
As an assessor, I look for the rhythm of treatment: examine, make a decision, discuss, prepare, provide, keep an eye on, reassess, file, turn over. When students internalise that loophole, their clients improve care and their stress goes down.
Common Risks and How to Avoid Them
A few patterns turn up repeatedly. The initial is dealing with discomfort scores as decoration rather than as decision supports. If the pain remains high after a reasonable start duration and there are no negative indications, titrate. If the discomfort drops to a mild degree, pivot to comfort actions and stop dosing. The second is equipment missteps: empty atomisers, expired vials, missing filters for inhalers. A pre‑shift list stops most of these. The 3rd is undervaluing non‑drug choices. Pain management is not a contest to see exactly how quickly you can formulate fentanyl. Splint early, train breathing, control the setting, after that reach for the vial.
The most major challenge is poor surveillance. A person who looks "comfortable adequate" can still move right into respiratory clinical depression, particularly in hot, enclosed rooms or during transportation when movement lulls them. Construct practices that endure distraction. Introduce your review breaks loud. Ask a teammate to establish a timer on the screen or phone. Write management times on your handwear cover if you must.
The Benefit: Faster Relief, Safer Treatment, Better Handover
When groups accept the complete extent of PUAEME008, scenes really feel various. Individuals relocate from panic to participation. Extrication times diminish since movement injures less. Transportation is calmer, handovers more clear. In audits, you will certainly see fewer outliers in dosing and a smoother spread of pain ratings trending down within 10 to 15 minutes pain management education courses of very first get in touch with for modest injury. The most effective praise I have gotten after an active event shift originated from a receiving registered nurse: "Your notes inform the tale, and the individual resembles the notes review."
If you are selecting a pain management certification program, concentrate on programs that rehearse the story from first call to handover instead of those that just educate how to push a medicine. If you manage a team, installed the device right into routine abilities upkeep. Pain management training for nurses, physiotherapists, and first -responders is not a one‑and‑done. Methods evolve and abilities boring without use. Quarterly short drills maintain the edge.
The heart of PUAEME008 is basic. Meet discomfort quickly and pleasantly, choose interventions that match the person and the scenario, enjoy carefully, and tell the next medical professional exactly what occurred. Do those things well and you will certainly fulfill the proficiency. A lot more significantly, you will certainly help individuals feel risk-free once more in mins that otherwise extend into an eternity.